Most dental practices assume that cutting supply costs means hunting for a new distributor or spending hours negotiating.
The reality is more straightforward and more frustrating, once you see it clearly.
Practices that run lean supply budgets are not doing anything exotic. They have built a system. They know what they buy, how much they use, and what it should cost across multiple sources.
That combination alone, applied consistently, can reduce supply spend by 30 to 40%.
Before getting into tactics, there is one metric worth anchoring to: supply spend as a percentage of revenue collections.
Try calculating this for your previous quarter. If your practice is running above 6.5%, something is off. For DSOs aiming for best-in-class performance, the target should be closer to 4 to 5%.
That single number captures everything: expired product, over-ordering, no price comparison, no preferred product list, no approval controls.
If you are above 6.5%, you do not need to guess where the money is going. You need a system that shows you.
Smaller practices or practice groups often assume they do not buy enough to get meaningful discounts. That belief keeps them from even trying.
Volume matters less than process. A single-location practice that runs a competitive quoting process, telling two or three suppliers "whoever has the lowest price wins the business", will consistently outperform a larger practice that sole-sources everything to one distributor.
Suppliers respond to competition. When a rep knows there is a fair process and a real shot at winning business, they bring their best pricing. When there is no competition, prices creep up slowly over time. The distributor knows they have the account. There is no pressure to stay sharp.
The fix is not switching vendors. It is adding one or two more to the conversation.
The goal is to keep two to three suppliers actively competing for your business, not more, not fewer.
More than four suppliers creates operational drag. Multiple invoices, multiple receiving events, multiple AP entries. The administrative cost starts eating the savings.
Fewer than two means no real competition, and prices will drift.
The process is simple. Put your preferred product list out to two or three suppliers at the same time, let them submit pricing, and award each item to whoever came in lowest. Lock pricing for three to six months, most suppliers will commit to this if they know they have a fair shot. Then repeat.
This is straightforward in theory and genuinely difficult to manage manually. Without software, tracking who quoted what on which item, assigning each product to the right supplier when placing the order, and monitoring whether locked pricing is being honored requires significant administrative effort.
That is why most practices do not do it consistently, even when they intend to.
None of the above works without a baseline of organization. Practices that waste the most on supplies are almost always the most disorganized, not because the staff is careless, but because there is no system telling anyone what is on the shelf, what gets used, or when to reorder.
When there is no system, ordering becomes reactive. Someone notices something looks low and places a rush order. Someone else already ordered the same thing last week. A case of something sits in the supply closet for eight months and expires.
Every dollar of expired or wasted inventory represents roughly four dollars of production needed to cover it. A $50 item that expires unused means the practice had to generate $200 in revenue just to break even on that one line item. Multiply that across a supply closet with no rotation system and the number gets uncomfortable.
A working inventory management process, even a basic one, prevents most of this. Know what you have, know what you use on average, and set a reorder point. An inventory tracking spreadsheet can do this for a smaller practice but for a truly effortless process, dental procurement software with barcode scanning makes it easy to place an order of what you need and no more than that.
Getting the lowest price on the product you already buy is only part of the picture. The deeper savings come from asking whether there is a comparable product, branded or private label, that delivers the same clinical outcome at a lower cost.
Not every product category works for this. Clinical items going in a patient's mouth deserve scrutiny. A dentist who prefers a specific composite or bonding agent for clinical reasons should not switch just to save money. But within many branded clinical products, there are comparable alternatives priced 20 to 30% lower from manufacturers with equally strong track records.
Non-clinical consumables, bibs, pouches, barriers, infection control supplies, are almost always safe territory for cost optimization with no clinical tradeoff.
The key is building a preferred product list that reflects both clinical standards and cost awareness, then sticking to it. Practices and DSOs that maintain this kind of list and update it when better options exist are the ones that hold their supply spend down year after year, rather than achieving a one-time savings and drifting back up.
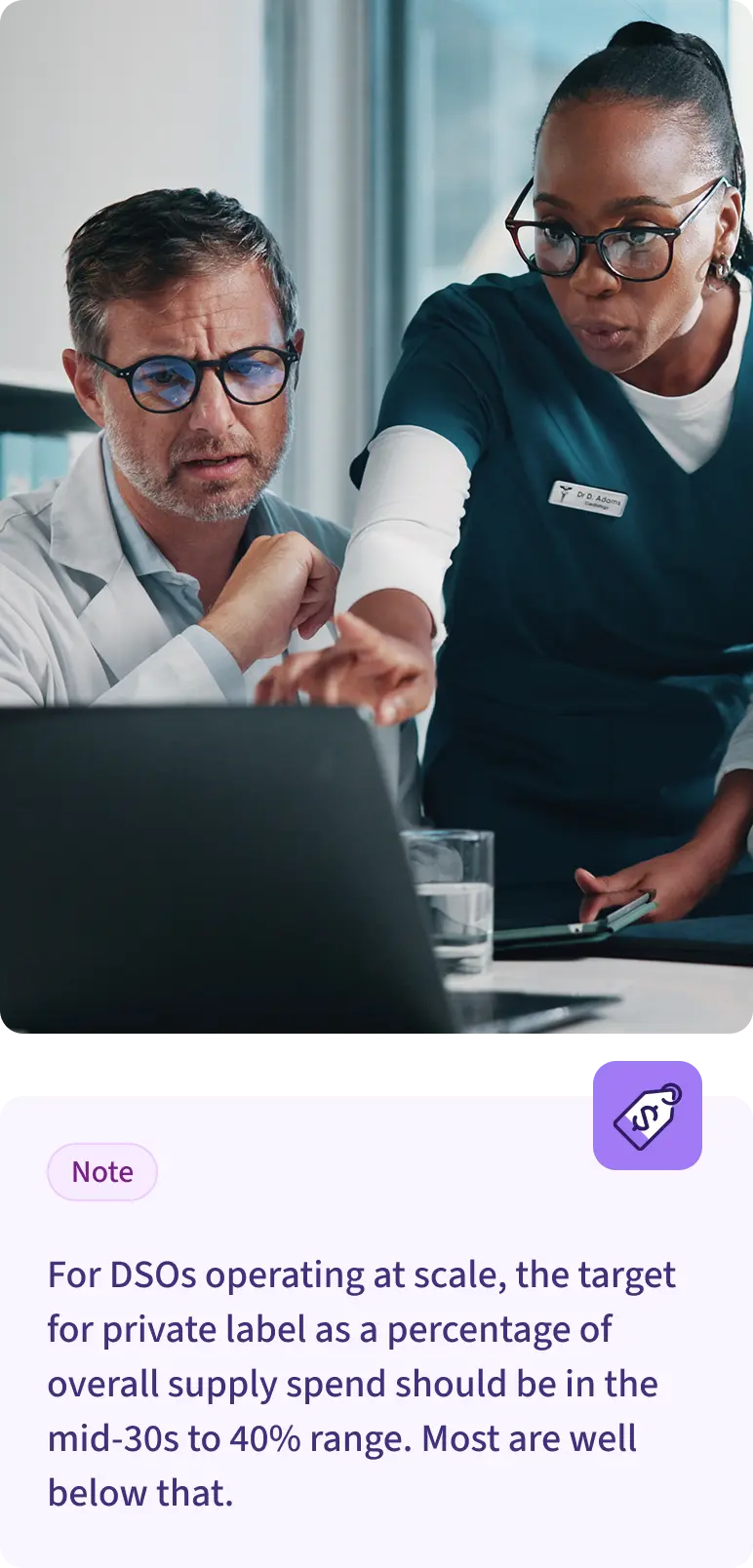
For DSOs operating at scale, the target for private label as a percentage of overall supply spend should be in the mid-30s to 40% range. Most are well below that.
Getting organized, finding the right products, and running a competitive process, in that order, will capture the majority of savings available to any practice.
The format of the system matters less than having one.
A paper-based reorder card system, a shared inventory spreadsheet, or dedicated dental procurement software can all work. What cannot work is no system at all, which is roughly where 30% of dental offices are today.
Method puts all three steps in one place: inventory tracking with barcode scanning, a preferred product list with formulary compliance tracking, multi-supplier quoting, and automated cost analysis that assigns each item to the lowest-priced supplier.
If your practice is running above 6.5% of collections on supplies, it is worth seeing what a structured process looks like in practice.









